12 Lead EKG: What It Measures and Why It Matters
12 Lead EKG: Reading, Interpreting, and What Abnormal Results Mean
A 12 lead EKG is one of the most widely used diagnostic tools in cardiology. It captures electrical activity from twelve different angles, giving clinicians a detailed picture of the heart’s function. An EKG heart attack pattern — such as ST elevation — can appear within minutes of a cardiac event, making fast interpretation critical. When results come back as EKG abnormal, that finding ranges from benign variants to serious arrhythmias. Preparing for an EKG exam requires understanding how each lead corresponds to a specific cardiac region. The EKG 12 lead configuration places electrodes on limbs and the chest to create a comprehensive electrical map.
Whether you’re a student studying for certification or a clinician brushing up on interpretation, the core principles remain consistent across settings.
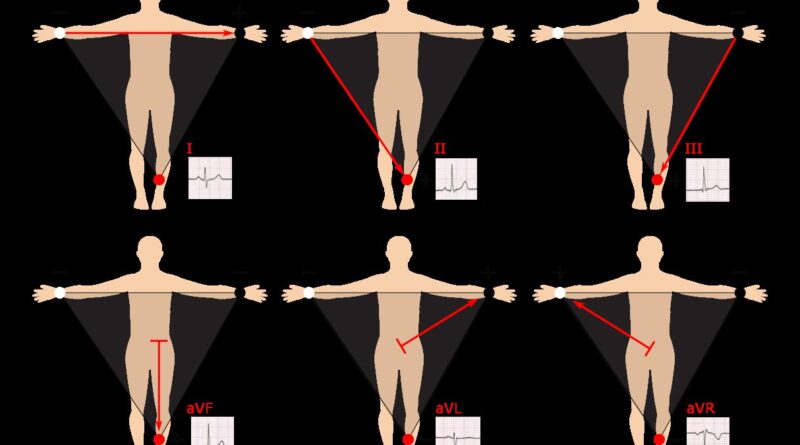
How a 12 Lead EKG Works
Each of the twelve leads records voltage differences between electrodes placed on the body. Limb leads look at the heart in a frontal plane, while precordial leads examine it horizontally. The combination gives a three-dimensional view no single lead can replicate. Performing the test correctly — proper placement, clean skin contact, and patient stillness — directly affects result quality. Running a twelve-lead cardiac tracing on a moving patient produces artifact that can mimic abnormalities.
Interpreting the resulting waveforms involves checking rate, rhythm, axis, intervals, and ST segments. Each parameter contributes to the overall clinical picture.
Recognizing EKG Heart Attack Patterns
The hallmark of a STEMI (ST-elevation myocardial infarction) is ST segment elevation in two or more contiguous leads. A cardiac event visible on a twelve-lead tracing typically shows reciprocal changes in opposing leads as well. Non-ST elevation events may show only T-wave inversions or subtle ST depression. Catching heart attack activity on an EKG early guides triage and treatment decisions within narrow time windows.
Common Causes of an Abnormal EKG
Not every abnormal cardiac tracing signals a heart attack. Bundle branch blocks, electrolyte imbalances, left ventricular hypertrophy, and benign early repolarization all produce unusual waveforms. An EKG finding described as abnormal requires clinical correlation — the tracing alone rarely tells the full story. Some patients carry abnormal baseline findings that are normal for them.
Preparing for an EKG Exam
Certification exams covering twelve-lead interpretation test knowledge of lead placement, waveform recognition, interval measurement, and arrhythmia identification. Studying rhythm strips alongside full twelve-lead examples builds the pattern recognition needed for exam success. Practice with varied cases — including normal variants — reduces the chance of over-calling benign findings.
Next steps: Focus your EKG study on systematic interpretation frameworks. Work through cases methodically: rate, rhythm, axis, hypertrophy, ischemia. Consistent practice with real tracings accelerates both exam readiness and clinical confidence.