Cervical Biopsy: What the Procedure Involves and What Your Results Mean
Cervical Biopsy: What the Procedure Involves and What Your Results Mean
A cervical biopsy removes a small amount of tissue from the cervix so a pathologist can examine its cells under a microscope. It’s typically ordered after an abnormal Pap smear or colposcopy finding, and it provides the definitive answer that a smear alone cannot — whether abnormal cells require treatment, monitoring, or no action at all. Understanding cervical biopsy results takes some specific vocabulary, and this article makes that vocabulary accessible.
We’ll also cover vulvar biopsy, vaginal biopsy, and eye biopsy — tissue sampling procedures that follow a similar logic but apply to different anatomical sites. Each serves a distinct diagnostic purpose, and knowing the differences helps you ask better questions when a provider recommends one.
What a Cervical Biopsy Involves
Types of Cervical Tissue Sampling
Several methods exist for obtaining cervical tissue, and the one your provider chooses depends on where the abnormal cells are located and how extensive they appear:
- Punch biopsy — A small circular instrument removes one or more tissue samples from the cervical surface. This is the most common type during a colposcopy visit.
- Cone biopsy (conization) — A cone-shaped section of tissue is removed from the cervix, capturing both surface and deeper cells. Used when abnormality extends into the cervical canal.
- Endocervical curettage (ECC) — A small curette scrapes tissue from inside the cervical canal, typically done alongside a punch biopsy.
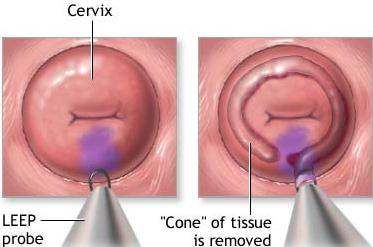
- LEEP (loop electrosurgical excision procedure) — A wire loop carrying electrical current cuts away tissue. Often both diagnostic and therapeutic in one step.
What to Expect During the Procedure
Most cervical tissue sampling takes place in a clinic setting without general anesthesia. You’ll lie in a standard gynecological position, and a speculum keeps the vaginal walls apart for access. A colposcope — a lighted magnifying instrument — helps the clinician identify abnormal-looking areas. The actual removal of tissue takes seconds per sample. Cramping similar to a menstrual period is common, and mild spotting may persist for several days. Avoiding tampons, sexual activity, and swimming for one to two weeks post-procedure reduces infection risk.
Understanding Cervical Biopsy Results
Normal vs. Abnormal Findings
A normal result means no precancerous or cancerous changes were found. Abnormal results are classified by the degree of cellular change. Interpreting cervical biopsy pathology reports requires understanding two classification systems: the older CIN system and the newer LAST/LSIL/HSIL terminology used increasingly in US pathology reports.
CIN Grades and What They Mean
CIN stands for cervical intraepithelial neoplasia — cell changes confined to the surface layer without invasion into deeper tissue.
- CIN 1 — Mild dysplasia. About 60–70% of CIN 1 lesions resolve without treatment. Most providers monitor with repeat testing.
- CIN 2 — Moderate dysplasia. Treatment is often recommended, particularly in patients over 25. Younger patients may be offered close surveillance given higher spontaneous regression rates.
- CIN 3 — Severe dysplasia or carcinoma in situ. Treatment is recommended because progression risk is significant.
Understanding cervical biopsy results also means knowing that HPV-related changes are the underlying cause of most abnormal findings, and that the same HPV strains detected in the cervix can affect the vagina and vulva — which is why additional tissue sampling may be ordered if colposcopy reveals abnormality at those sites.
Vulvar and Vaginal Biopsy: How They Differ
Vulvar Biopsy: Purpose and Process
A vulvar biopsy removes tissue from the external genitalia to evaluate lesions, persistent itching, discoloration, or ulcerations that don’t respond to topical treatment. The area is numbed with a local anesthetic, and a small punch tool or scalpel removes tissue — the procedure typically takes under 10 minutes. Results diagnose conditions including vulvar intraepithelial neoplasia (VIN), lichen sclerosus, lichen planus, contact dermatitis, and rarely invasive carcinoma. Vulvar tissue sampling is generally less uncomfortable than cervical procedures because local anesthesia blocks pain effectively at that site.
Vaginal Biopsy: When It Is Ordered
Vaginal tissue sampling addresses lesions on the vaginal wall, which are often identified during colposcopy when the scope is slowly withdrawn. Vaginal intraepithelial neoplasia (VAIN) is the most common indication, though infectious lesions, cysts, and polyps may also be sampled. The vaginal wall has fewer nerve endings than the vulvar area, so discomfort is usually minimal with local numbing.
Eye Biopsy: A Different Tissue, A Similar Principle
An eye biopsy applies the same core principle — remove tissue, examine it microscopically — to ocular structures. It’s far less common than gynecological tissue sampling and is ordered when imaging and other non-invasive tests cannot definitively characterize a lesion. Indications include suspected ocular melanoma, lymphoma involving the choroid or conjunctiva, orbital mass of uncertain origin, and certain inflammatory conditions not responding to empirical treatment.
Depending on the lesion location, an ocular biopsy may sample the conjunctiva, vitreous fluid, choroid, or orbital tissue. Fine-needle aspiration biopsy is frequently used for intraocular lesions to minimize trauma and preserve vision. Incisional biopsy — removing a wedge of tissue — is used for accessible conjunctival or orbital lesions. The results guide decisions about radiation, chemotherapy, or surgical removal, making accurate tissue diagnosis essential before committing to treatment.