PD Catheter Placement: What Patients and Nurses Need to Know
PD Catheter Placement: What Patients and Nurses Need to Know
Peritoneal dialysis starts with a critical step: pd catheter placement, the surgical procedure that creates access to the peritoneal cavity. This differs from dialysis catheter placement for hemodialysis, which targets a blood vessel rather than the abdominal lining. Understanding catheter dialysis access types helps patients and care teams make informed decisions about the right modality. A pd catheter belt is a wearable accessory that protects the exit site and keeps the catheter secure during daily activity. For nurses entering this specialty, dialysis nurse training covers both the clinical and technical aspects of managing patients on peritoneal therapy.
How PD Catheter Placement Is Performed
Surgical and Bedside Techniques
PD catheters are placed using three main methods: open surgical insertion, laparoscopic placement, and percutaneous (bedside) insertion. Open surgery provides direct visualization and is preferred when adhesions or prior abdominal surgeries complicate access. Laparoscopic placement offers faster recovery and lower infection risk. Percutaneous dialysis catheter placement can be done at the bedside under fluoroscopic guidance, though it carries a higher misplacement risk. Most nephrologists prefer laparoscopic peritoneal catheter insertion for newly diagnosed patients who need time to heal before starting dialysis.
The Exit Site and Break-In Period
After placing a catheter for dialysis, the exit site requires careful management during a two-to-four-week break-in period. No full immersion bathing is permitted, and the site must be cleaned daily using sterile technique. The break-in period allows fibrous tissue to anchor the catheter, reducing the risk of leaks. A properly healed exit site dramatically lowers long-term infection rates, which is a central focus of dialysis nurse training programs covering PD access care.
Using a PD Catheter Belt for Daily Management
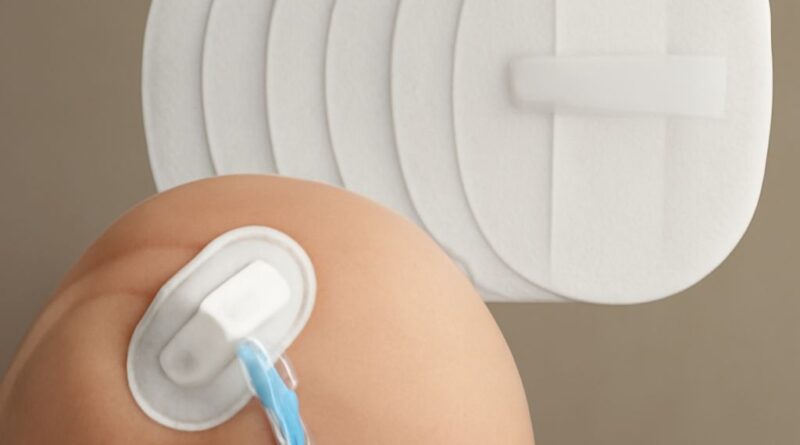
A pd catheter belt wraps around the abdomen to hold the catheter tubing flat against the skin. This prevents tugging at the exit site during movement and reduces trauma to the tunnel tract. Belts are typically made of soft, breathable fabric and are available in sizes to accommodate different body types. Wearing a catheter belt for peritoneal dialysis consistently—especially during physical activity—extends catheter function life. Nurses teaching self-care during dialysis nurse training programs should demonstrate proper belt fitting as part of exit site education.
Dialysis Nurse Training for PD Catheter Care
Dialysis catheter nursing competencies include aseptic technique for connections and disconnections, exit site assessment, recognition of early infection signs, and troubleshooting flow problems. Dialysis nurse training programs cover both hemodialysis and peritoneal access, though PD-specific training emphasizes patient independence since most catheter dialysis patients manage treatments at home. Nurses entering renal care should seek facilities with structured PD orientation programs that include supervised catheter care practice. Key takeaways: PD catheter placement technique affects long-term outcomes, exit site care during the break-in period is non-negotiable, a catheter belt reduces mechanical trauma daily, and dialysis nurses need PD-specific training to prepare patients effectively for home therapy.